We know that people have different blood types. What this means is some people have one “factor” and some don’t. Some have A, and some have B, and some don’t have either. We call them type A, B and O (think of “zero” if it helps). If you needed a blood transfusion you would have to get it from someone who has the same blood factors which you have — or else from someone who doesn’t have those blood factors, someone who is type “O” (without A or B). If you were given the wrong blood, your body would attack and destroy the new blood like a foreign invader — and you would get very sick very quickly.
A baby in the womb can be a different blood type from the mom because the blood very rarely mixes — and there is a natural mechanism, which usually protects both mom and baby if it does occur. The baby has completely different blood supply from the mom — and the mom’s body doesn’t reject or attack the baby even though his blood and tissue are “foreign” to her.
Well. .. aside from the major blood group, there are minor factors and proteins as well as the major ones, A and B. One of them is the Rh factor (called “Rh” because the first researchers were using “Rhesus” monkeys when they were trying to find out why some babies were being damaged in their mother’s wombs). A baby in the womb can have the same or a different blood type from his mom, and there won’t be problems — but some of the “minor factors” like “Rh” MIGHT cause problems.
A mom who is Rh “negative” doesn’t have the Rh factor. She might be type A, B or O, and is called “negative” if she lacks Rh. (She will be either A-, B- or O-).
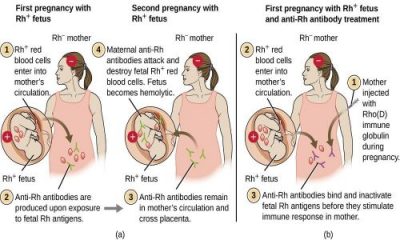
If she gets pregnant with a baby who also doesn’t have the Rh-factor (an Rh-negative baby) then there is no problem. But if she gets pregnant with a baby who DOES have a blood type with Rh (an Rh-positive baby) then there might be problems. If there is any mixing of the mom’s and baby’s blood — as often happens during birth or sometimes in late pregnancy — then the mother’s body may make antibodies to destroy the “foreign invaders” – the Rh-positive blood cells. This process is similar (though much slower) to what might happen if someone were given the wrong type of blood during a blood transfusion.
This baby is usually born before the mom’s body can make this response, so there is no harm to this baby. But the NEXT time she becomes pregnant with an Rh-positive baby, the mom’s body may attack the new baby by sending these antibodies’ through the placenta and destroying the baby’s red blood cells. This can cause serious anemia — and if it goes on long enough can even cause the baby’s death.
We can protect the mom’s future babies by giving the mom an injection of Rhogam shortly after any birth of an Rh-positive baby — before her body has a chance to make antibodies to any Rh-positive blood cells which might have gotten mixed in her circulation during the birth. The next time she gets pregnant with an Rh-positive baby, it will be just like the first time — there won’t be any Rh-antibodies already formed waiting to attack the new baby in the womb.
A woman who is Rh-positive DOES have the Rh factor/protein. If she gets pregnant with an Rh-positive baby, then her blood already has this Rh factor and there will be no problem. If she gets pregnant with an Rh-negative baby, there will still be no problem, since the body mounts an immune response only if it detects a “foreign” factor. The Rh-negative baby has no factors to trigger the mother’s antibody response.
Sometimes are terms are confusing. When we call a mom “Rh-negative” it doesn’t mean she has a different type of Rh than the mom who is “Rh-positive”. It means she has NO Rh factor — no “rhesus factor”. This is why her body reacts when it detects the Rh factor from her baby — or from the wrong type of blood transfusion. She makes antibodies to the blood cells, which are “incompatible” with her own blood type. If a mom carries an Rh-negative baby, there will be no Rh-factor cells to trigger a response. And if mom is Rh-positive, she can safely carry a baby with any blood type — the Rh factor is not an issue at all for her. Her husband’s blood type isn’t important either since it doesn’t matter whether her babies will be Rh-positive or Rh-negative.
The father’s blood type is important only if a mom is Rh-negative. Her baby will inherit a blood type from her husband. The Rh factor is a dominant gene. If the mother is Rh-negative, it means she has no rh factor and can only contribute a gene with an Rh-negative blood type; therefore her husband’s genes will be responsible for the blood type of the baby.
If the father is also Rh-negative, then all their babies will also be Rh-negative. There will never be a problem with Rh-disease in their pregnancies. But if the father is Rh-positive then this means he has the Rh factor and can father Rh positive babies, though he still “might” carry a recessive Rh-negative gene. (There is a blood test to discover this).
If he is Rh-positive but does not carry the recessive gene, then every one of their babies will be Rh-positive and at risk of Rh-disease. But if he carries the Rh-negative recessive gene, then there is a chance that some of their children will be Rh-negative, and also that some will be Rh-positive (but carry the recessive gene like their father).
This is why we test a mom’s blood to discover her blood type and her Rh factor. If the mom is Rh-positive, she never has to worry about developing a Rh blood incompatibility with her babies. But if we find she is Rh-negative, we also test her husband’s blood type as well. If she is Rh-negative and her husband is also Rh-negative, then there is no risk of having an Rh problem with their babies. Only if she is negative and if her husband is Rh-positive, will there be a risk of their babies developing an Rh- problem!